LRC director MARIANA FIGUEIRO lays out the smart play for progress in human-centric lighting, or lighting for health and wellbeing, which is to integrate intelligent data-collection functionality with lighting to enable customized circadian lighting.
The Internet of Things (IoT) is here to stay. Everyone is now connected to something — a phone, a tablet, a computer, even a light bulb. And the number of IoT-connected devices is growing rapidly. A recent study by market researcher Gartner conservatively estimates that the number of connected “things” worldwide in 2017 will more than double by 2020, increasing from about 8.4 billion devices to 20.4 billion devices, with more than 60% of the growth being attributable to consumer products and services. Lighting already plays a key role in this networked world because it provides an essential service in every space that is connected to the IoT. Realizing that the luminaire is perfectly suited to IoT infrastructure, the lighting industry has capitalized on this developingopportunity.
With the IoT in place, we can now track individuals’ locations in buildings, discern what they are doing, suggest products that they might need (or don’t yet know they need), adjust the indoor environment to provide comfort (visual, thermal, air quality, etc.), calculate energy use, and a host of other tasks. The result is that we now have multiple sensors following us in multiple ways, generating “big data” that can interface with myriad systems operating on vastly different scales. But to what end will the data be used, and for what real value? What can lighting contribute to these rapidly evolving and increasingly complex systems?
Light and health: Biology basics
We should keep in mind that lighting is not simply a conduit for gathering and conveying information, and that we light spaces for many reasons. Light reaching the retina allows us to see effectively and efficiently, helps us navigate through the built environment, creates an atmosphere, and helps to minimize the risk of falls.
More to the point at hand, though, light also regulates the timing of our biological clock and thereby affects our sleep, alertness, health, and general wellbeing. Yet light’s effect on these outputs of the biological clock is perhaps the most complex and least understood aspect of lighting.
Biological rhythms that repeat about every 24 hours are called circadian rhythms, and light is the main stimulus that synchronizes them with the solar day. The human circadian system is driven by a series of biological clocks located in cells throughout the body, which are controlled by a master biological clock seated in the hypothalamus region of the brain. The master biological clock is stimulated by light received on our retinas, and research has found that we need to be exposed to a sufficient amount of light in the right spectrum for a sufficient amount of time and at the right time to remain synchronized with the solar day.
A lack of synchronization can have negative effects on our physiological functions, neurobehavioral performance, and sleep. When experienced over long periods of time, as can happen with rotating night-shift workers, desynchronization has been associated with more serious health conditions such as diabetes and obesity, and increased risk for cardiovascular disease and cancer.
The lighting characteristics that affect the circadian system are different from those that affect visibility. Melatonin is a hormone we produce at night and in darkness and tells our body that it is nighttime. Circadian effects are measured by acute suppression of melatonin and shifts in the timing (or phase) of its production. Even low levels of light, for example, can affect the body’s melatonin production, but those levels are still higher than the light levels that are required to affect vision.1,2Humans are “blue sky detectors” because the peak sensitivity for acutely suppressing and shifting the phase of human melatonin production is close to 460 nm.3-5
The effects of light-exposure types impact the circadian system in various ways at different times of the day. “Morning” light experienced after the trough of core body temperature (one of our circadian rhythms), which typically occurs in the second half of the night, will advance the timing of sleep in the following cycle. On the other hand, “evening” light experienced prior to the trough of core body temperature will delay the timing of sleep.6
Closely connected with the timing of exposure is one’s cumulative history of light exposures over the 24-hour day. Research has shown that measuring this history is far more informative than simply taking a measurement of light exposure at one certain place and time.7,8 As the circadian system appears to closely monitor light exposure, tracking the unique patterns of light and dark experienced over the past 24 hours can help determine the best lighting prescription for the next 24 hours (Fig. 1).9 Therefore, while the spectrum and timing of light exposures are very important factors, lighting that aims to promote circadian synchronization (also known as entrainment) should also keep track of time and control the total circadian light exposure during waking hours.
FIG. 1. Solid-state lighting (SSL) products combined with the behavioral data-tracking applications of the IoT can deliver healthy home lighting that supports circadian rhythms with appropriately-timed morning (top) and evening (bottom) light settings.
Lighting impact studies
Initial studies of light’s therapeutic application focused on treating the symptoms of seasonal affective disorder (SAD). While the mechanisms associated with light’s beneficial effects on SAD are not yet well established, physicians nonetheless recognize light as a therapy and recommend it as a sole or adjunct treatment for SAD. But conventionally-prescribed light therapy boxes, which are very bright and glary, can unfortunately reduce patients’ compliance with the treatment and thereby reduce its efficacy. Newly-developed, more effective technologies such as solid-state lighting (SSL) have permitted the development and use of better targeted, less glary solutions for relieving SAD symptoms.
Most of the other published laboratory and field research to date has examined lighting for office workers, older adults with Alzheimer’s disease and related dementias (ADRD), and adolescents. Multiple studies have attempted to demonstrate the benefits of lighting that provides higher circadian stimulation in the built environment during the daytime, with some studies also employing a reduction in circadian stimulation during evening hours. Researchers generally agree that lighting schemes for daytime workers should be designed to promote circadian entrainment, which in turn should result in better sleep, mood, health, and perhaps performance. Additional research has also examined how light can be used to increase alertness, without regard to its impact on circadian phase. This is particularly relevant for night-shift workers, who need to be alert at work but also should avoid disrupting their melatonin cycle.
A recent Lighting Research Center (LRC) study in five office buildings showed that office workers who received high circadian stimulation in the morning reported better sleep and fewer depressive symptoms than those who received low circadian stimulation in the morning. While the importance of reducing evening light exposures to maintain a regular sleep–wake cycle is already widely known, this study also demonstrated the benefit of providing good circadian stimulation throughout the entire workday.
Field research focused on older adults with ADRD has shown that a lighting intervention providing high circadian stimulation during the day and low stimulation at night reduced depressive symptoms among those living at home. In nursing homes, where light exposures are more easily controlled, the same intervention resulted in improvements to sleep, depression, and agitation. In another LRC study conducted in a nursing home, a lighting intervention with very high circadian stimulation was delivered to residents using a specially-designed LED light table. Residents who sat around the table, as residents conventionally do in nursing-home common areas, showed significantly increased sleep duration and reduced agitation and depression scores.
Adolescents can be chronically sleep deprived because they are unable to fall asleep early and face fixed wakeup times on school days, which has been linked to depression, behavioral problems, poor performance at school, and automobile accidents. This problem can be compounded by adolescents spending most of their day indoors in dimly-lit classrooms, which inhibits the synchronization of their circadian systems with the solar day, followed by the use of self-luminous electronic devices in the evening, which can delay their circadian phase. Studies by the LRC have pointed to the importance of controlling the entirety of 24-hour light–dark patterns to effectively promote circadian entrainment and reduce sleep restriction inadolescents.
Apart from sharing the circadian system’s response to patterns of light and dark, these divergent populations have very little in common, and lighting interventions to improve their health and wellbeing defy a one-size-fits-all solution. Yet that is precisely why and how the IoT can play a vital role!
The IoT’s role in light and health
Current research shows that it is important to tailor lighting systems to meet the circadian needs of the people who occupy any given space. Control schedules for adolescent students will be different from those for ADRD patients in nursing homes, and those for US Navy submariners will be different again from those for night-shift nurses, who might themselves be attending to premature infants in a neonatal intensive care unit whose lighting needs are also distinctly different. But how do we meet these needs?
One example of how the IoT and lighting for healthy outcomes can work together is a current joint research project involving the LRC, Lund University, and the Swedish Energy Agency. For this project, called the Swedish Healthy Home, we assumed that individual homes are the most effective places for making lighting adjustments to promote healthy outcomes. Because most people have limited control over the lighting they experience in public buildings such as workplaces or schools, the home serves as the hub for a healthy life, essentially by default. However, using home lighting to promote good health requires that we track and record light exposures throughout the day, understand how that light interacts with our biological systems, and then make the necessary lighting adjustments. All these measures would be virtually impossible to carry out on one’s own, even for the vast majority of people in the world’s most-developedcountries.
A technology that can track, record, and interpret light exposure lies at the core of the project. A device — in this case, the Daysimeter developed by the LRC (Fig. 2) — tracks each household member’s light exposure throughout the day and transmits the data for storage on a smartphone or other portable electronic device (PED). Upon arrival at home each day, the data are then automatically transmitted to the home’s central lighting control system, providing the basis for an individualized home-based lighting plan for each person. This system tailors and administers a personalized lighting treatment from the time someone walks through the door to the time they leave the next day.
FIG. 2. A small, wearable tracker like the LRC’s Daysimeter is a key component in a tailored smart lighting system that delivers scheduled lighting schemes based on individual user data.
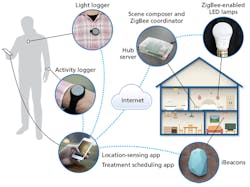
For the system to work effectively, the Daysimeter (or a similar device) must be worn at all waking times, whether inside or outside the home. As the person moves from room to room, the home’s lighting system recognizes the personal device and dynamically adjusts the lighting to provide an intervention specified to counterbalance the light exposures received outside the home (Fig. 3). If the system’s automatic controls are undesirable at any time and for any length of time, the system can be overridden and configured to provide notifications of lighting needs and measures to be taken via residents’ personal PEDs.
Image credits: The Swedish Energy Agency, Lund University, IAI Inc., and LRC.
FIG. 3. The Swedish Healthy Home project infographic provides one example of how the various devices and hardware interact in an IoT-based system to adjust to the user’s lighting needs.
As most Americans do not live alone, according to the US Census, it’s easy to imagine a situation where conflicting lighting needs among multiple household members might lead to situations akin to battles over the television remote control in the days of single-television homes. The lighting system designed for this project, however, is configured to adjust the lighting in a particular area of a room to best suit individual needs. Should this not be possible because several people are grouped in one area at the same time, the system can use a preset hierarchy to select a lighting intervention suited to the person most in need of circadian adjustment or most sensitive to circadian disruption (or the parents can have the final decision!). The system would also send a notice to the PEDs of those whose lighting needs might be imperiled by the chosen lighting intervention, advising them to use personal light “dosing devices” or filtering devices such as light goggles or spectrally-filtered glasses.
In this way, the lighting intervention and any appropriate countermeasures provided by the Daysimeter system would help to entrain the circadian system of every household member, every day, and thereby promote their health and wellbeing. Because the system is dynamic and portable, it would also be easily translated to one’s schoolroom orworkspace.
Obstacles to an IoT role in health and wellbeing
The principal challenge for the lighting industry is to break free from thinking about lighting a particular building as a static, standalone entity where one primarily needs to see for task performance and perceive ambience instantaneously. Research suggests that conventional lighting schemes in the built environment that deliver dim, constant light over the course of the 24-hour day can be associated with disruption of the human circadian system and elevated risks for sleep disturbances and reduced general wellbeing. For circadian health, lighting must follow everyone from building to building and make adjustments over the entire course of the 24-hour day. The IoT holds great promise for finally realizing comprehensive, circadian-healthy lighting systems that do just that. Successful circadian lighting systems are those that can deliver and remove circadian-effective light at the right time, not just those that can tune the spectrum. It is about time!
With the implementation of the appropriate hardware infrastructure and software applications that track light–dark exposures and administer light treatments for maintaining entrainment or correcting circadian disruption, the IoT could provide virtual, 24/7 personal light and health coaching for end users. Over time, thanks to constant and consistent monitoring by IoT technology, circadian lighting systems could eventually learn users’ behavior and automatically program the lighting over the long term, freeing them from the need to wear their personal sensors. The sensors could be put away until users feel that they need a tune-up or temporarily recycled for the benefit of other users.
Why should the lighting industry take the lead?
The benefits of lighting that helps us sleep, improves our mood, reduces depression, or makes us feel more alert on the job are, simply put, priceless. What parent of an autistic child would not pay a premium for a 24-hour lighting system that would reduce the need for pharmaceutical sleep aids? What family would hesitate to purchase a new table lamp that would help a beloved grandparent remain at home rather than move to an assisted living facility? What employer would not upgrade the workplace lighting system, knowing that it would increase employee alertness and wellbeing at work?
With the IoT in place and rapidly growing in terms of distribution and capability, the lighting industry is in an excellent position to realize healthy lighting technology for all and to continue to improve IoT technology. If the industry does not articulate the value of circadian-healthy lighting beyond the four walls of static spaces or beyond tunable lighting systems, however, it will not be in the driver’s seat.
REFERENCES
1. A.J. Lewy et al., “Light Suppresses Melatonin Secretion in Humans,” Science, 210, 1267–9, 1980.
2. J.M. Zeitzer et al., “Sensitivity of the human circadian pacemaker to nocturnal light: melatonin phase resetting and suppression,” J. Physiol., 526, 695–702, 2000.
3. G.C. Brainard et al., “Action spectrum for melatonin regulation in humans: evidence for a novel circadian photoreceptor,” J. Neurosci., 21, 6405–12, 2001.
4. K. Thapan et al., “An action spectrum for melatonin suppression: evidence for a novel non-rod, non-cone photoreceptor system in humans,” J. Physiol., 535, 261–7, 2001.
5. M.S. Rea et al., “A model of phototransduction by the human circadian system,” Brain Res. Rev., 50, 213–28, 2005.
6. S.B. Khalsa et al., “A phase response curve to single bright light pulses in human subjects,” J. Physiol., 549, 945–52, 2003.
7. M.S. Rea et al., “A new approach to understanding the impact of circadian disruption on human health,” J. Circadian Rhythms, 6, 7, 2008.
8. M.G. Figueiro et al., “Comparisons of three practical field devices used to measure personal light exposures and activity levels,” Light Res. Technol., 45, 421–34, 2013.
9. M. Figueiro et al., “Daylight exposure has a positive carryover effect on nighttime performance and subjective sleepiness,” Light Res. Technol., 46, 506–19, 2014.
MARIANA G. FIGUEIRO, PhD, is director of the Lighting Research Center at Rensselaer Polytechnic Institute (lrc.rpi.edu).
Further reading on human-centric lighting
The Lighting Research Center (LRC) certainly has a lot to offer on additional human-centric lighting resources from its own website publications archives — some of which are included below — but LRC director and author Mariana Figueiro has also incorporated some excellent external resources in this reading list. ◀
- R. Blau, “The Light Therapeutic,” The Economist: Intelligent Life, 2014.
- M.G. Figueiro, “Illuminating the importance of lighting design,” TEDMED, 2015.
- M.G. Figueiro, “Light Therapy for Better Sleep,” Sleep Rev., 2015.
- M.G. Figueiro, “The Value Proposition: Where are the Products?” Lighting Design + Application (LD+A), 2014.
- M.G. Figueiro, K. Gonzales, and D. Pedler, “Designing with Circadian Stimulus,” Lighting Design + Application (LD+A), 30–34, October 2016.
- Lighting Research Center Light & Health Website.
- M.R. Smith and C.I. Eastman, “Shift work: health, performance and safety problems, traditional countermeasures, and innovative management strategies to reduce circadian misalignment,” Nature and Science of Sleep, 4, 111–132, 2012.
- F.W. Turek, “Circadian clocks: Not your grandfather’s clock,” Science, 354, 6315, 992–993, 2016.
- M.S. Vitaterna, J.S. Takahashi, and F.W. Turek, “Overview of circadian rhythms,” Alcohol Res. and Health, 25, 2, 85–93, 2001.
Editor's note: References were condensed for space in the magazine. Full author details are shown in the outbound links.